Saving Your Skin
Prevention and treatment for frostbite.
Physiologically, humans are tropical beings, better suited to losing heat than retaining it. When naked and at rest, a person's neutral environmental temperature is 28°C (82°F)… In comparison, the Arctic fox can maintain a steady thermal state within an external temperature of -40°C (-40°F) .
—McCauley, Robert, et al, in Wilderness Medicine, 4th Edition, Paul Auerbach, Editor., p. 178.
For those of us going outdoors year-round in Montana, the unhappy consequences of this physiological fact are hypothermia and frostbite. As we’ve discussed in previous issues, hypothermia occurs when our core temperature drops, usually the result of being both cold and damp. Hypothermia is a progressive systemic condition which, when unrecognized and untreated, can lead to loss of mental function and eventually death. Frostbite, on the other hand, is a localized cold problem. Our core temperature may be just fine and we may be having a great day at our pastime of choice—our life is not in jeopardy, but our limbs are.
In order for our human ancestors to cope with the tropical 82-degree temperature in which they lived, they had (and we also have) an excellent radiator built in—our skin. We can increase the amount of blood routed to our skin 30 fold to lose excess heat. Unfortunately, we have a poor ability to cope when the weather turns cold. That’s why our ice-age ancestors wore furs over their poly underwear.
As skin temperature (here we go being naked and at rest again) decreases from 82 degrees, the blood vessels in our skin begin to constrict, reaching maximum constriction at 59 degrees. Colder than this, a complex response is triggered, designed to save our lives by losing less heat, but still saving our skin (literally). Since the body’s core shares some heat with the overlying skin, the skin temperature can decrease to 25 degrees before it actually freezes. When the skin does freeze, it’s frostbite.
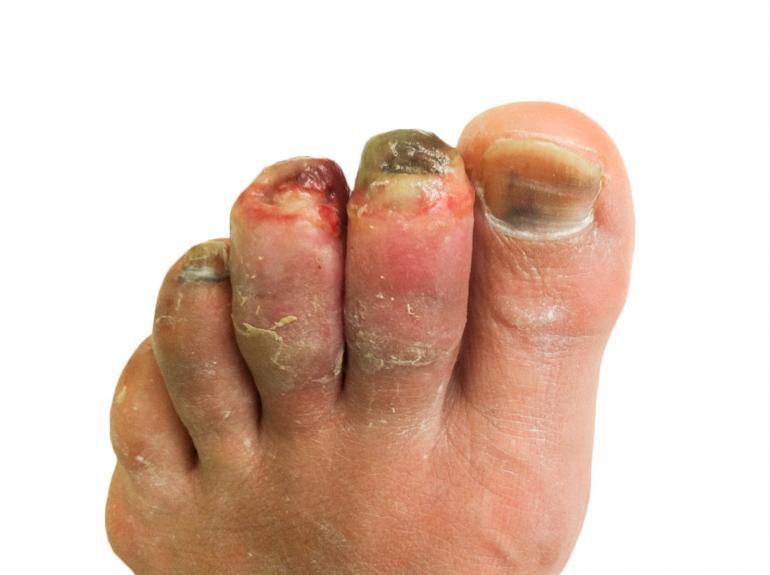
To characterize the amount and nature of damage from frostbite and predict ultimate tissue loss, frostbite is divided into two types: superficial and deep. Superficial frostbite begins with redness; then a white, firm patch develops as the damage increases. Caught at this level of severity and re-warmed, there is seldom any permanent tissue loss. A blister may form; followed by a scab that later comes off, leaving temporarily sensitive, but otherwise normal, skin.
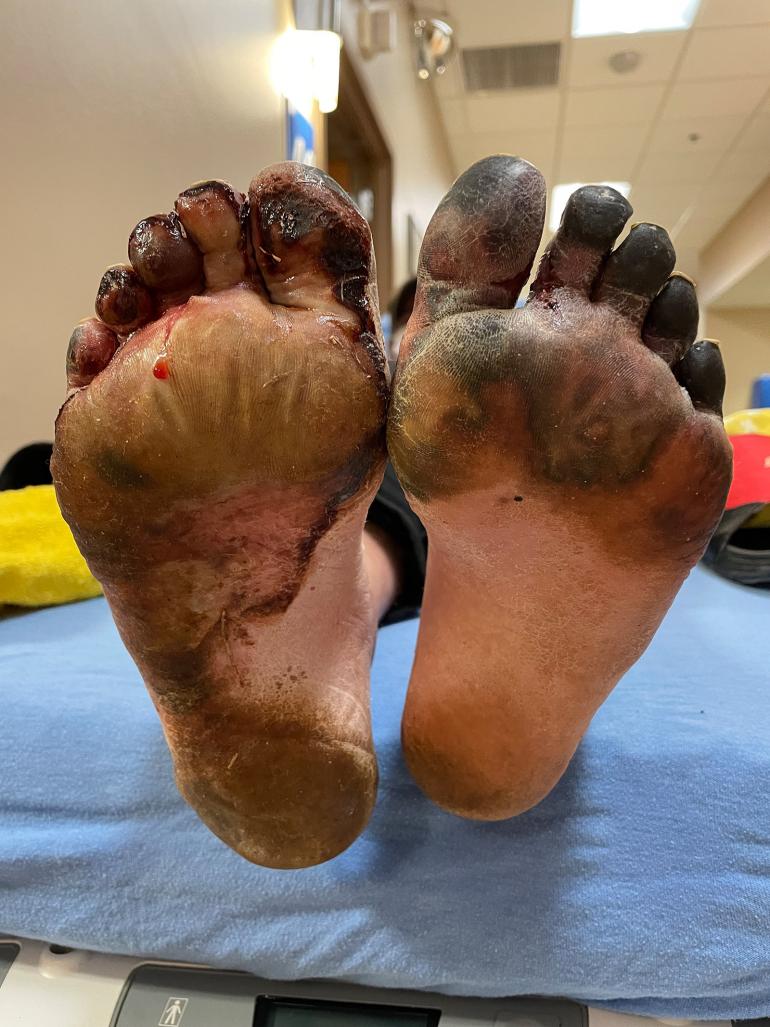
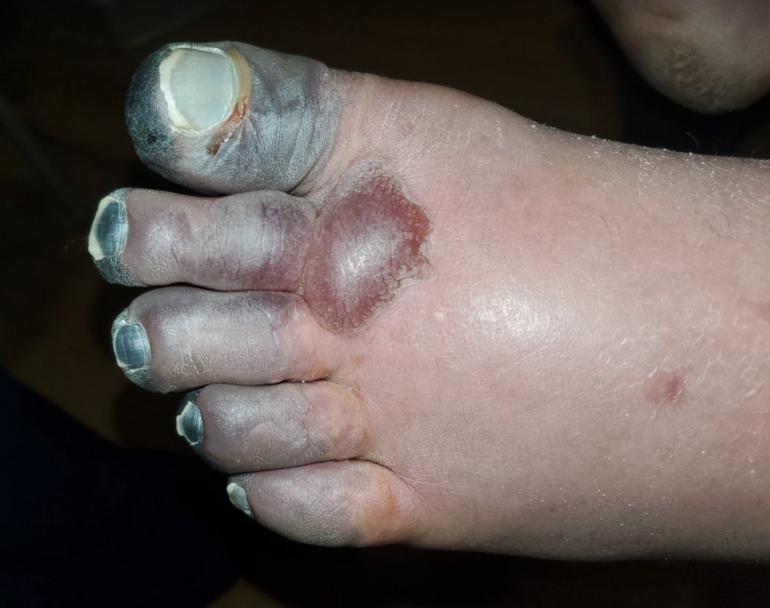
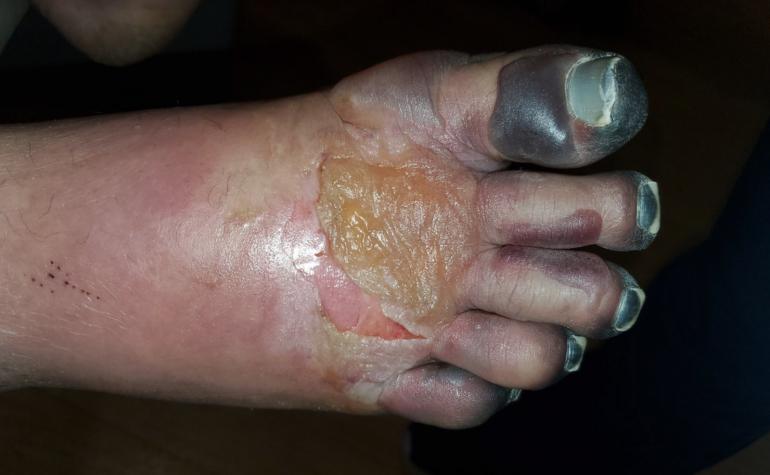
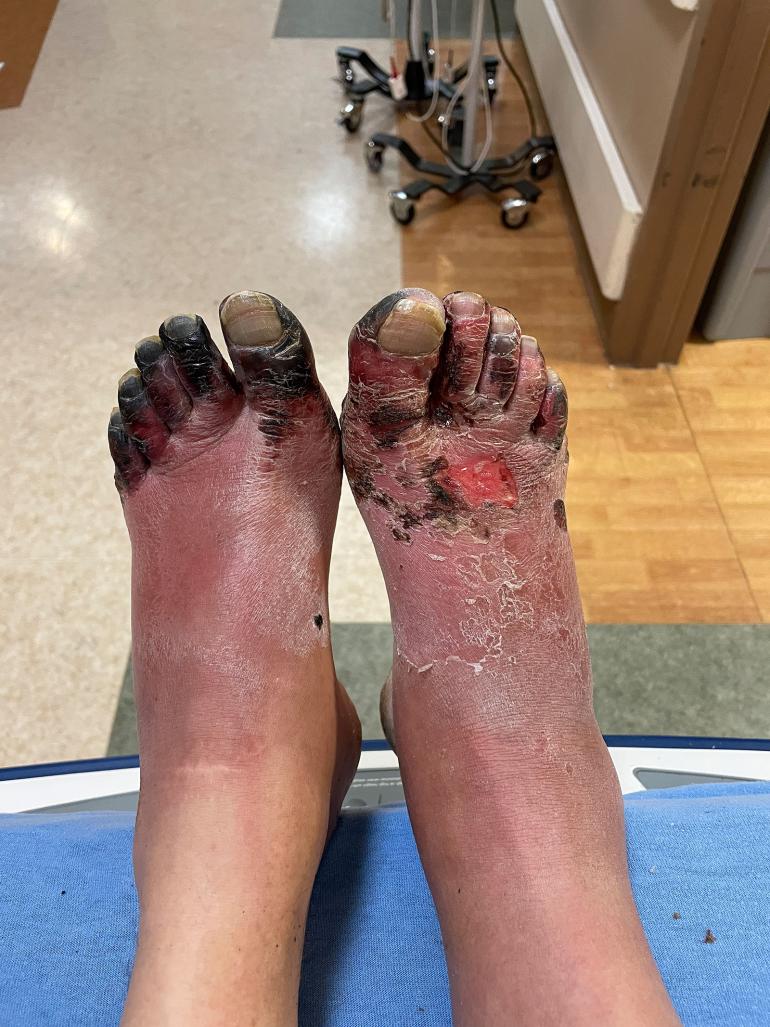
If the freezing continues longer, the injury goes deeper, causing damage to the full thickness of the skin. If the freezing continues longer still, fat, tendons, nerves, and muscles below the skin may be damaged. Deep frostbite causes blisters (often with blood in them), and whole parts may be gray-white and lifeless-looking. After re-warming, these injuries throb painfully for days. Deep frostbite is very difficult to assess at first, and it takes weeks to see how much loss of tissue, disfigurement, and function occurs.
The best treatment for frostbite, like most medical problems, is prevention. If you’re outdoors when the air temperature is below 20 degrees, dress properly and plan for surprises with extra clothing and emergency gear. Remember that wind increases the risk at any temperature. The parts that stick out get less heat from the core below and are the most sensitive to frostbite, so make sure you have them covered. (As Dr. Seuss might say, “Fingers, toes, ears, nose. These are hurt when winter blows.”) And remember that fashionable is usually dumb. Wear mittens and a hat that covers your ears. Have a facemask, scarf, or wide neck warmer. Footgear fit and warmth are critical.
The next best treatment is close observation of yourself and your companions. Since our skin goes numb at 50 degrees skin temperature, we don’t feel the damage occurring—one has to look. If an exposed area of skin becomes red, or a white patch forms, get it warm as soon as possible. Since refreezing dramatically increases the extent of freezing damage, don’t let the area freeze again. Do not follow old, harmful advice by rubbing the area (especially with snow), toasting your skin like marshmallows over a fire, or drinking alcohol.
If you’re way out in the backcountry and injury, equipment failure, or poor route-finding leave you in trouble, you’ll have to make the decision to re-warm a frozen part or leave it frozen. If skilled help is within two hours, and the victim is not hypothermic, it should probably be left frozen. If you are more than two hours from help, there are very limited circumstances where re-warming in hot-tub-temperature water might be the right answer. If you can’t re-warm or prevent refreezing, try to limit damage by replacing wet clothing and loosening any that is tight-fitting, then padding and splinting the frozen part.
Keep in mind that re-warming frostbite is painful, so try not to need it.
Dean Center, M.D. is a physician at Family Doctors' Urgent Care in Bozeman, 556-9740.